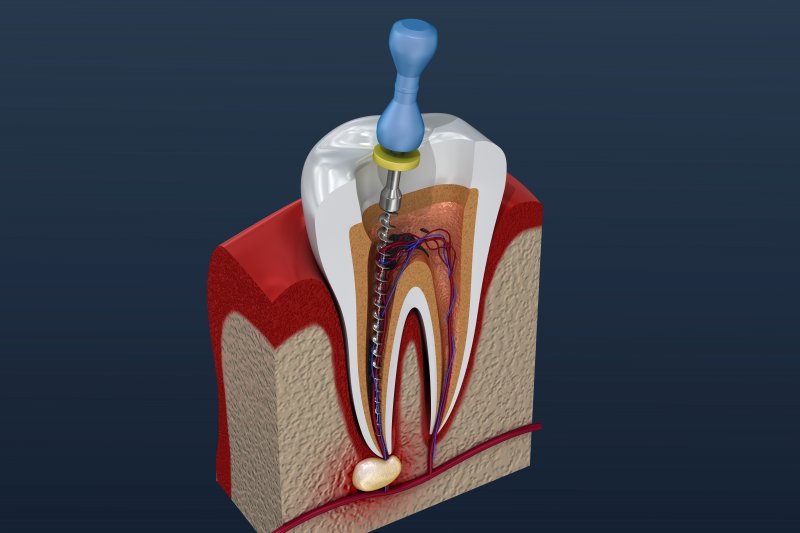
A root canal treatment, also known as endodontic therapy, is a dental procedure to treat infection at the center of a tooth. It is not a painful procedure, despite common myths. The treatment is necessary when the soft tissue inside the root canal becomes inflamed or infected. Here is more information on the procedure, common misconceptions, and what the process involves:
What Is a Root Canal?
A root canal is an anatomical space within the root of a human tooth. It contains the dental pulp, a soft tissue that houses nerves and blood vessels. The term also refers to the specific dental procedure used to treat infection within this space, and dentists perform this treatment to preserve the natural tooth structure.
The pulp tissue plays a central role during the early development of a tooth. Once the tooth is fully mature, it can survive without the internal pulp. The surrounding tissues provide adequate nourishment, and the tooth continues to function normally. This physiological reality makes the treatment an effective long-term solution for patients.
How Does It Work?
The treatment works by removing infected or damaged pulp from the interior of the tooth. A specialist accesses the inner chamber and then carefully extracts the compromised tissue. The empty space is then cleaned to remove bacteria and remaining debris. The practitioner fills the canal with a biocompatible material to seal it completely.
Why Is It Conducted?
Dentists conduct this procedure to address deep decay or traumatic injury to a tooth. When bacteria penetrate the outer enamel, the inner pulp becomes heavily infected. An untreated infection leads to an abscess, or it can cause severe bone loss around the root. Removing the infected tissue stops the spread of bacteria and preserves the patient’s natural bite.
What Does the Process Involve?
The clinical process begins with a thorough examination and diagnostic dental X-rays. A local anesthetic is applied to numb the area, and specialized instruments are used to open the crown and clean the root canals. The space is shaped, then filled with a rubber-like material called gutta-percha.
After the root canal is filled, a temporary filling is placed to close the opening. Patients usually return for a second appointment, and the dentist places a permanent crown on the tooth. This final restoration protects the remaining tooth structure from further damage. It restores the tooth’s full structural function, and it allows the patient to chew normally.
What Are Myths and Facts?
Several misconceptions surround this specific endodontic procedure. Some people believe the treatment is highly painful, but modern anesthesia makes it comparable to receiving a routine filling. Another common myth claims that extracting the tooth is a better clinical option. Retaining the natural tooth maintains proper jaw alignment, preventing the need for artificial replacements.
Some individuals think the procedure causes illness in other parts of the body, but there is no scientific evidence to support this claim. The treatment actually eliminates localized infection before it can spread systemically through the bloodstream. Understanding these facts helps patients approach their dental care with accurate expectations.
Consult an Endodontic Specialist Today
A root canal treatment effectively removes internal infection and restores normal dental function. Misinformation may surround the procedure, but clinical evidence demonstrates its safety and success. The clinical steps involve precise cleaning, sealing, and protecting the affected tooth. Contact a local endodontic clinic to schedule a professional evaluation.