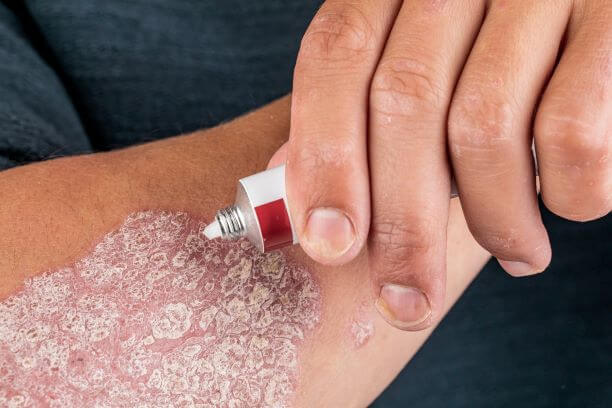
A dermatologist is a specialized doctor who treats complex skin conditions, and they provide relief for patients facing psoriasis. Psoriasis is a chronic autoimmune disease. Because this illness causes rapid skin cell buildup, it leads to painful scaly patches on the body. Doctors create tailored management that soothes irritated skin to improve your daily comfort and long-term health.
Understanding Dermatologist Roles
A dermatologist evaluates your skin, and they diagnose various skin-related medical conditions. They treat severe issues like skin cancer and more mild ones, such as eczema. When patients notice unusual rashes, these medical professionals conduct thorough examinations to find the root cause of the irritation.
Doctors prescribe medications for stubborn acne, and they perform minor surgical procedures in their clinics. General practitioners may refer patients to these specialists. Dermatologists educate patients about proper skincare routines for their unique skin and circumstances. Since environmental factors can harm the skin, doctors recommend protective measures to prevent future damage.
Exploring Psoriasis Causes
Psoriasis is a chronic autoimmune condition. The immune system mistakenly attacks healthy skin cells, and this abnormal process speeds up the life cycle of the skin. While normal skin cells grow over a month, cells affected by psoriasis can multiply in days.
Researchers study genetic links to psoriasis, and they believe family history plays a role in the development of the condition. Certain triggers can also worsen the disease unexpectedly. When patients experience heavy stress or severe infections, their skin may react aggressively to the environmental changes.
Cold weather dries out the skin, and this sudden climate change worsens painful flare-ups. Smoking is another known environmental trigger that can worsen the effects of psoriasis. Alcohol consumption may affect immune responses. Doctors may advise patients to limit their daily intake of alcoholic beverages.
Identifying Psoriasis Symptoms
Patients experience diverse physical symptoms of psoriasis. Red patches of skin are very common. Because these patches feature thick silver scales, they look distinct from ordinary dry skin patches. The scales may itch, and when a patient scratches, it potentially detaches the scales and causes bleeding.
When the disease affects the fingernails, the nails become pitted or detach from the nail bed entirely. The skin feels incredibly itchy, and it burns during severe outbreaks. You might experience joint problems. These issues indicate a related condition called psoriatic arthritis.
Watch for the following warning signs of this condition:
- Swollen or stiff joints
- Pain radiating through the lower back
- Changes in normal nail texture
If you notice these symptoms, a medical professional can evaluate your overall health.
Administering Psoriasis Treatments
Doctors prescribe topical treatments, and patients apply these specialized creams directly to the skin. Corticosteroids reduce inflammation. Since vitamin D supplementation may slow down skin cell growth, doctors include it in a daily care routine.
Salicylic acid promotes peeling. When thick scales resist other medications, salicylic acid softens the skin to help other treatments penetrate deeper into the affected areas. Retinoids come in gel form, and they decrease skin cell production.
Learn More About Psoriasis
Psoriasis causes uncomfortable skin patches, and a skin specialist helps manage this chronic condition effectively. These doctors diagnose the root causes of your skin-related symptoms to provide targeted treatments. Because they offer targeted treatments like creams and steroids, patients may find lasting relief from their painful psoriatic symptoms. If you want to learn more about psoriasis treatment, consult a dermatologist near you.