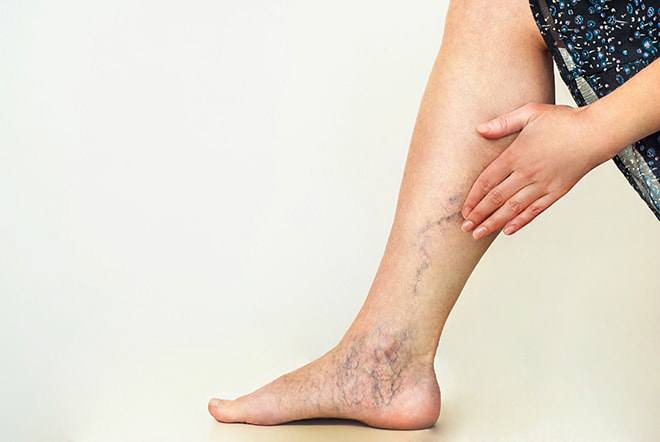
Varicose veins are visible under the surface of your skin. These veins may form clusters, and they often appear blue or purple. Changes in vein elasticity can affect healthy blood flow. Learning how to manage this condition helps support comfort and mobility while understanding your risks.
Understanding Causes and Risk Factors
Several factors contribute to changes in the veins. Normal aging can stiffen vein walls, and excess weight adds vascular pressure. Genetics may play a part, but daily lifestyle choices play a role, so staying active is recommended. Sitting or standing for long periods decreases circulation. Extended standing increases physical pressure, and this can strain your veins. You may inherit this condition, and family history influences your personal risk. Work environments that require standing or sitting for hours might contribute to over time. While age weakens vein valves, healthy habits support your circulation. Certain health conditions may raise venous pressure. Some women have higher hormonal risks.
To help prevent vein-related issues, adopting healthy lifestyle habits provides benefits. Regular physical activity, such as walking, promotes blood circulation and strengthens vascular health. Elevating your legs periodically, especially when sitting or standing for extended periods, helps reduce pressure on your veins. Maintaining a healthy weight and balanced diet reduces unnecessary strain, while staying hydrated supports overall vascular function. Wearing compression stockings may provide additional support, so ask about them if you are experiencing symptoms. Your provider may have recommendations. Avoid prolonged immobility, whether sitting or standing. By integrating these practices into your routine, you actively support your vascular health and reduce potential risks.
Recognizing Symptoms and Complications
Varicose veins may lead to heavy or tired legs, and this affects your activity level. Legs can ache, and ankles swell during the day. Over time, visible, bulging veins or spider veins can appear on your legs. Skin discoloration and venous ulcers can develop if symptoms are not addressed. Some cases are associated with blood clot formation. Superficial thrombophlebitis causes local pain. Deep vein thrombosis requires evaluation by a professional, and early steps may help. Itching can occur around the affected veins. Leg muscles cramp, and throbbing pain can disturb sleep. Because blood clots sometimes move, clinicians monitor patients for pulmonary embolism. Some people report restless legs. Skin around the veins may be sore.
Exploring Treatment Options
Medical professionals provide several vein treatment options. Doctors assess your veins, and they suggest appropriate non-surgical therapies. Medical technology continues to improve, offering more approaches to care, and some procedures reduce swelling. Radiofrequency ablation uses targeted heat to close veins. Sclerotherapy focuses on small spider veins, while endovenous chemical ablation treats larger vessels. These minimally invasive methods usually require little downtime, and many people return to normal activities soon after treatment. Treatments target the affected vein sections directly. Healing times vary, but most experience little disruption to their daily routine. People often explore these treatments to address pain or mobility concerns. The recovery period is typically short. Specialists help suggest a care plan that fits your needs.
Treat Varicose Veins Today
Preventive steps support your vascular health over time. Try wearing compression stockings and elevate your legs each day. Because prolonged sitting reduces blood flow, taking breaks to walk and move is recommended. Regular activity, supportive clothing, and attention to daily routines help you maintain comfort.