The hair growth cycle consists of distinct phases of activity and rest. Some individuals experience disruptions in this cycle, which may lead to noticeable hair thinning. Hormonal fluctuations are a primary factor in this process, so understanding this connection helps patients make informed decisions about their care. Here is more information on hair loss and the available medical treatments:
What Is Hair Loss?
Hair loss is a clinical condition characterized by the reduction of hair density on the scalp or body. The medical term for this condition is alopecia, and it affects both men and women across different age groups. The standard growth cycle includes the anagen, catagen, and telogen phases. Hair falls out during the telogen phase, but the follicle typically generates a new hair shaft shortly after.
What Causes It?
Multiple physiological and environmental factors disrupt the standard hair growth cycle. Genetics plays a significant role in pattern baldness, and autoimmune responses can lead to conditions like alopecia areata. Nutritional deficiencies limit the resources available for follicular development. Medical therapies sometimes induce hair shedding, and severe physical stress pushes follicles into a premature resting phase.
What Are the Symptoms?
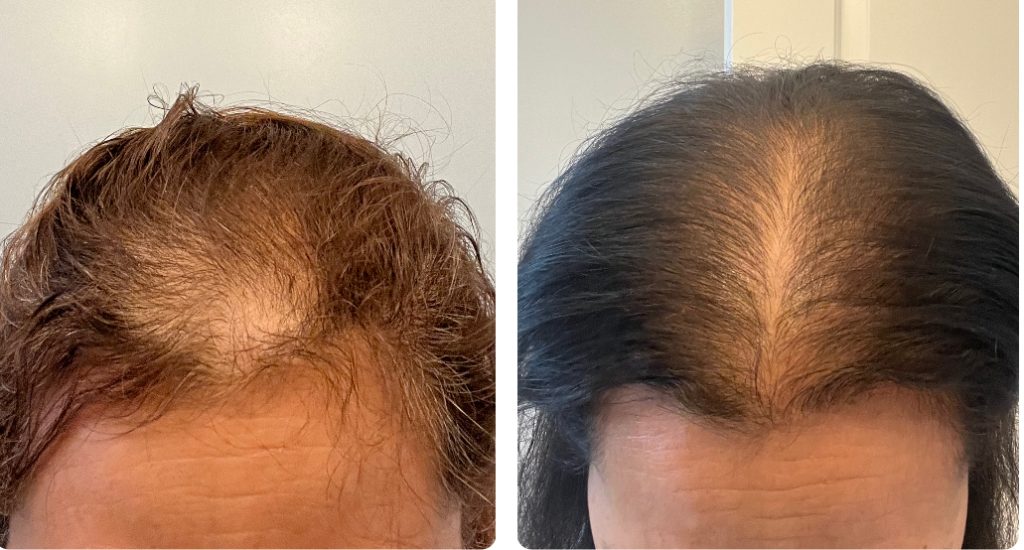
Patients present with a variety of physical signs when experiencing alopecia. Gradual thinning on the top of the head is a common symptom, and it may present differently in men than in women. Some individuals notice sudden hair loosening during washing or brushing. Patchy bald spots may appear on the scalp, affecting the patient’s quality of life.
How Do Hormones Affect Hair Loss?
Fluctuations in the endocrine system affect the lifecycle of individual hair follicles. Androgens may bind to receptors in the scalp, and this action shrinks the follicles over time. The anagen growth phase shortens, making hair strands thinner and more fragile. Thyroid imbalances also disrupt the growth cycle.
Estrogen and progesterone typically prolong the active growth phase of hair. A drop in these hormone levels triggers shedding, which may occur during postpartum recovery or menopause. The body loses the protective effect of these hormones, so the influence of androgens becomes more pronounced. These hormonal shifts require medical evaluation for accurate diagnosis.
What Are the Treatment Options?
Medical science offers multiple therapeutic approaches for managing hormone-related alopecia. Regenerative medicine utilizes stem cells and exosomes to stimulate follicular activity. Clinicians extract these components, and they inject them directly into the affected areas of the scalp. These cellular signals promote tissue repair, so dormant follicles may resume active hair production.
PRP therapy involves extracting and concentrating platelets from the patient’s own blood. Medical professionals draw a small sample, and a centrifuge separates the required plasma. The concentrated plasma contains growth factors, so injections into the scalp stimulate hair follicle regeneration. This protocol may involve multiple sessions spaced over several months.
Bioidentical hormone replacement therapy addresses the specific endocrine imbalances causing hair loss. Medical providers administer hormones that match the molecular structure of naturally occurring hormones, thereby restoring systemic levels. Regulating these levels reduces the negative effects of DHT, so hair follicles can return to a normal growth cycle. Regular monitoring keeps hormone levels within safe clinical ranges.
Consult a Specialist Today
Understanding the relationship between hormones and hair loss aids in effective intervention. Individuals experiencing alopecia have access to various medical therapies, but an accurate diagnosis is key. A medical evaluation identifies the specific hormonal factors at play, which guides the selection of an appropriate treatment plan. Schedule a consultation with a clinical provider today to discuss your specific symptoms and review your treatment options.