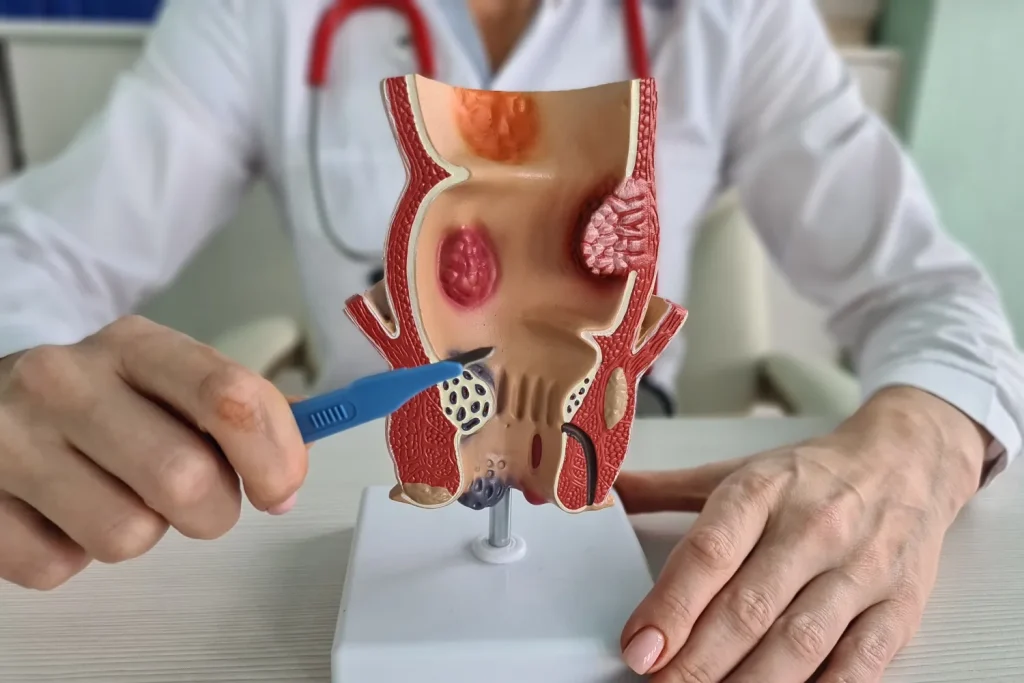
Hemorrhoids involve swollen blood vessels in the lower rectum, and patients experience varying levels of physical discomfort. Understanding the medical facts provides clarity about the condition, enabling individuals to make informed decisions regarding their personal healthcare. Here is more information on this condition, its causes, symptoms, and when to seek professional help:
What Are Hemorrhoids?
Hemorrhoids are naturally occurring vascular structures in the anal canal that help with stool control. These structures become problematic when they swell, and doctors refer to this abnormal state as hemorrhoids. Medical professionals categorize severity based on the location of the swelling.
Internal hemorrhoids lie deep inside the rectum, and patients cannot typically see or feel them. These internal structures rarely cause pain, but passing stool can irritate their delicate surface. External hemorrhoids lie under the skin around the anus, an area that contains highly sensitive nerve endings. Blood can occasionally pool in an external hemorrhoid and form a clot.
What Causes Them?
Increased pressure in the lower rectum causes these veins to swell. Straining during bowel movements is a primary cause, and chronic constipation may lead to this excess strain. Sitting on the toilet for extended periods increases downward pressure, stretching the local blood vessels. The veins lose their elasticity over time, causing them to bulge.
Pregnancy places weight on the pelvic region, and this extra weight presses heavily on the anal veins. Obesity also increases pelvic pressure. A low-fiber diet produces hard stools that are more difficult to pass. Aging weakens the tissues that support the veins in the rectum, making the vessels more susceptible to swelling.
What Are the Symptoms?
Patients with hemorrhoids experience a specific set of physical indicators, and these signs vary based on the type of hemorrhoid. Painless bleeding during bowel movements is common, and individuals may notice bright red blood on their toilet tissue. Itching or irritation in the anal region may occur, leading to further scratching and tissue damage. Swelling around the anus creates physical discomfort.
What Are the Treatment Options?
Medical professionals utilize several methods to treat hemorrhoids. The chosen approach depends on the severity of the symptoms. Infrared coagulation (IRC) involves applying intense heat to the affected tissue, which cuts off the blood supply to the hemorrhoid. The lack of blood flow causes the swollen vein to shrink, and the surrounding tissue eventually heals.
Rubber band ligation is another clinical intervention that effectively treats internal hemorrhoids. A physician places small rubber bands around the base of the hemorrhoid, cutting off the local circulation. The banded tissue withers, and it ultimately falls off. This procedure may provide long-term relief.
Severe cases require more invasive surgical procedures, and a hemorrhoidectomy is a comprehensive option. A surgeon removes the excess tissue causing the bleeding. This surgical method helps with severe hemorrhoids, and the recovery period requires careful medical supervision. Patients follow specific post-operative instructions, which promote tissue healing.
When Should You Seek Help?
Patients should consult a medical professional if their symptoms do not improve after a week of home care. A prompt medical evaluation rules out other serious conditions, improving colorectal health. Rectal bleeding requires immediate clinical assessment, as it can indicate diseases other than hemorrhoids. A doctor will examine the area thoroughly to establish an accurate medical diagnosis.
Seek Professional Help Today
Hemorrhoids may cause physical discomfort, and they disrupt basic daily routines for some patients. The medical field offers multiple effective treatments, including procedures like infrared coagulation that provide lasting clinical results. Delaying a medical evaluation can worsen the condition. Call a local medical center to set up an initial consultation.