Palliative care focuses on patient comfort. Medical teams use interventions to manage symptoms, so doctors use cryoablation for this exact purpose. Cryoablation uses extreme cold to destroy abnormal tissues. Because tumors cause discomfort, specialists apply targeted freezing.
Treatment Fundamentals
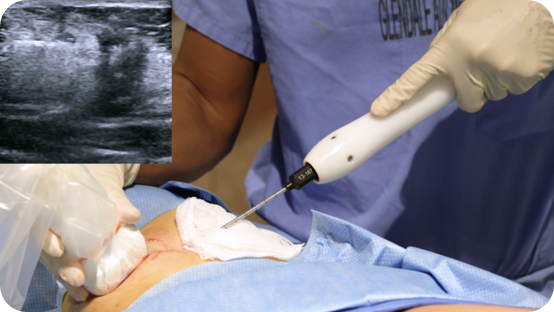
Cryoablation addresses specific cancer types in the body. Specialists insert thin probes into the targeted areas. The probe reaches lung tumors, and argon gas cools the tip. This process causes minimal disruption to the surrounding tissues. The procedure typically uses only local anesthesia and sedation rather than general anesthesia, which helps reduce risk. Ultrasound guides the medical tools during the procedure. Imaging technology aids precise needle placement. Doctors view ice formation in real time, and they protect healthy surrounding tissues from unnecessary damage. Providers use CT scans for greater precision. Recovery after cryoablation is often quicker than after open surgery, which involves longer hospital stays. The frozen tissue thaws naturally, and the body gradually absorbs dead cells. Physicians adjust the approach for each individual, and they tailor the procedure to the patient’s needs.
Organ Applications
Medical professionals may apply cold therapy to different areas. This approach also treats tumors in the kidney, lung, chest, and liver. The treatment targets cervical cancer lesions, and similar techniques are available for some other tumors. Freezing interrupts tumor growth and numbs the affected area, providing relief. In kidney tumor cases, cryoablation sometimes allows preservation of healthy kidney tissue. This offers an option for those who are not candidates for certain surgeries. When large masses press on organs, doctors use freezing to interrupt nerve activity. Some patients return home the same day.
Imaging guides the procedure, and it enhances precision. Interventional radiologists and oncologists use cryoablation for chest, liver, or kidney tumors. Localized cooling reduces bleeding during and after the procedure. It also helps limit swelling. Providers monitor the internal temperature throughout the procedure. This protects healthy surrounding tissue, and it avoids frostbite. When treatments finish, providers carefully remove the probes. The puncture site heals over several days with minimal scarring. In some cases, scar tissue forms over the treated cervical areas or at the site of other tumors. The healing process varies for each individual and takes several weeks. Many people notice a gradual return to comfort and daily routines within days.
Recovery Protocols
Patients usually return home the same day, especially when local anesthesia is used. Mild soreness at the treatment site is common and often managed with standard pain relief, while stronger medications are rarely required. Some people experience mild bruising or swelling near the area, which resolves within a week. If minor bleeding is noted, providers typically apply pressure and resolve the situation without further intervention. Doctors and nurses give clear instructions about what to watch for at home, such as increasing pain or persistent redness around the area. Follow-up imaging checks the initial results, and it monitors the tumor. These scans confirm the treatment outcome, and it allows the provider to assess comfort levels. Because palliative goals focus on comfort, care plans are tailored to each person’s needs and preferences.
Book Palliative Cryoablation Today
Discuss this medical option with your primary doctor, so they can evaluate your specific physical condition. Write down your questions, and bring them to your appointment. If you need tumor symptom relief, ask about cryoablation. Review the potential medical benefits together. Every patient differs, so personalized medical advice is necessary. Gathering information helps you understand your choices and make informed decisions.