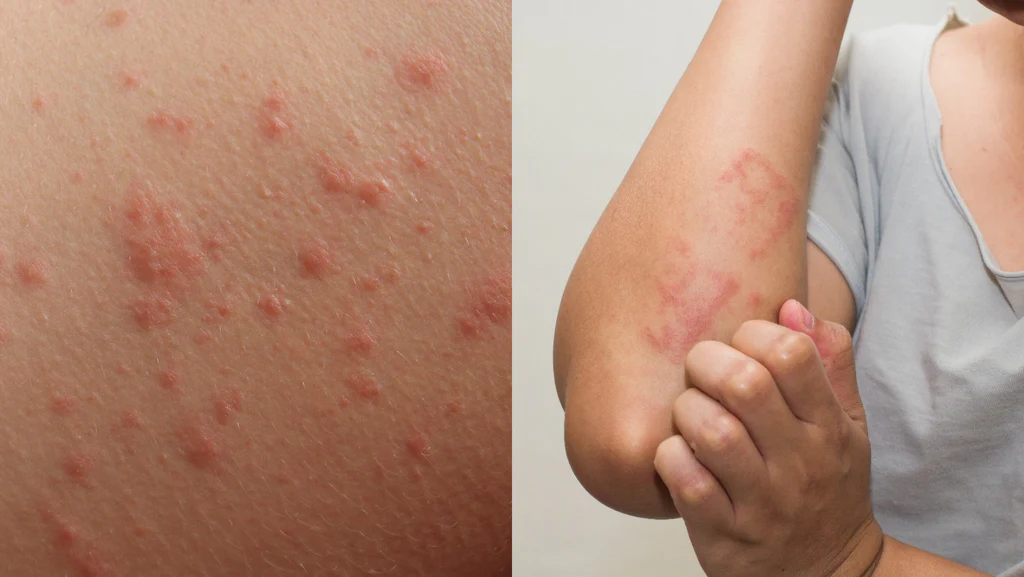
Eczema refers to a group of conditions that cause the skin to become irritated, inflamed, or itchy. This condition can appear at any age, and it manifests in various ways depending on the individual. While many people use the term interchangeably with a specific type of skin rash, there are several distinct types of eczema. Identifying the correct type is a step in understanding your skin and maintaining daily wellness.
Comprehensive Understanding of Eczema
Eczema is a broad term used to describe various skin conditions, and it affects millions of people worldwide. At its core, eczema often involves an impaired skin barrier. When the skin barrier is compromised, it struggles to retain moisture effectively and becomes more susceptible to external irritants. This dynamic leads to the characteristic dryness and irritation that many people experience regularly.
Managing eczema typically requires a consistent, gentle skincare routine to help support the skin’s natural barrier. Individuals frequently need to identify specific environmental factors that aggravate their skin, such as harsh soaps, extreme weather, or certain fabrics. Some triggers are easy to avoid, but others require more careful daily management. Understanding your unique skin responses is a helpful step toward finding a sustainable daily care routine.
Common Types of Eczema
Certain variations of this condition appear more frequently than others. Recognizing the specific visual characteristics of these common types helps you better understand your skin’s ongoing needs, and it can also guide you in choosing appropriate skincare routines. By becoming familiar with how these forms often present, you can take more informed steps toward supporting your skin health.
Atopic dermatitis is the most prevalent form of eczema; it typically begins in childhood, though adults can develop it as well. Individuals with atopic dermatitis often experience chronic dry skin, along with rashes that frequently appear in the creases of the elbows or behind the knees. Recognizing these specific areas and patterns can support your understanding of this common type.
Contact dermatitis occurs when the skin comes into direct contact with a specific substance. It is divided into two main categories: allergic contact dermatitis and irritant contact dermatitis. The physical reaction usually appears strictly in the area where the substance contacted the skin, and this makes identification focused on localized patches of irritation. Understanding what causes these reactions can help you take practical steps to reduce your exposure and manage symptoms.
Less Common Types of Eczema
Atopic and contact dermatitis are widely recognized, but several other forms present with distinct characteristics. You can experience small blisters on your hands or develop circular patches on your arms. These unique patterns and symptoms sometimes require a closer look to understand what type of eczema may be present.
- Dyshidrotic Eczema: This type primarily affects the extremities. It presents as small, deep-seated blisters on the palms of the hands, the soles of the feet, and the edges of the fingers and toes.
- Nummular Eczema: Also known as discoid eczema, this variation features distinct, coin-shaped patches of irritated skin. These circular spots are often raised and scaly and can sometimes occur after a minor skin injury.
- Seborrheic Dermatitis: This form commonly appears in areas of the body with a high concentration of oil glands, such as the scalp, upper back, and the sides of the nose. On the scalp, mild cases are frequently recognized as common dandruff.
Ask a Dermatologist Today
Since different forms of eczema share similar visual characteristics, accurate identification by a trained professional is recommended. Dermatologists are physicians with specialized training in the diagnosis and management of skin conditions. If your skin concerns persist or begin to impact your daily routine, scheduling a professional consultation is advisable. A specialist can evaluate your skin history, and they are able to provide clear, precise information about your specific situation. Ask your dermatologist any questions about your triggers or management strategies.